A step-by-step daily routine for acne-prone skin. Gentle cleansing, targeted actives, barrier protection, and the habits that keep breakouts from coming back.
Why Your Routine Matters More Than Any Single Product
You have tried spot treatments. You have bought expensive face washes. You have watched videos about miracle ingredients. Your skin still breaks out.
The problem is rarely the product. The problem is the system. Or the lack of one.
Acne responds to consistent, daily routines built around a few proven principles: gentle cleansing, targeted active ingredients, barrier protection, and sun protection. No single product clears acne on its own. The combination of the right steps in the right order, repeated daily, is what produces results.
The American Academy of Dermatology recommends a structured daily routine as the first-line approach for mild to moderate acne. Dermatologists estimate that 85% of people between the ages of 12 and 24 experience acne. About 15% of adult women deal with acne past the age of 25. The condition is not rare. Effective home care makes a measurable difference for the majority of these cases.
This guide gives you a complete daily routine. Morning steps. Night steps. The specific products to use. How to layer them. What to avoid. And the habits that keep your skin clear between applications.
How Acne Forms (And Where Your Routine Intervenes)
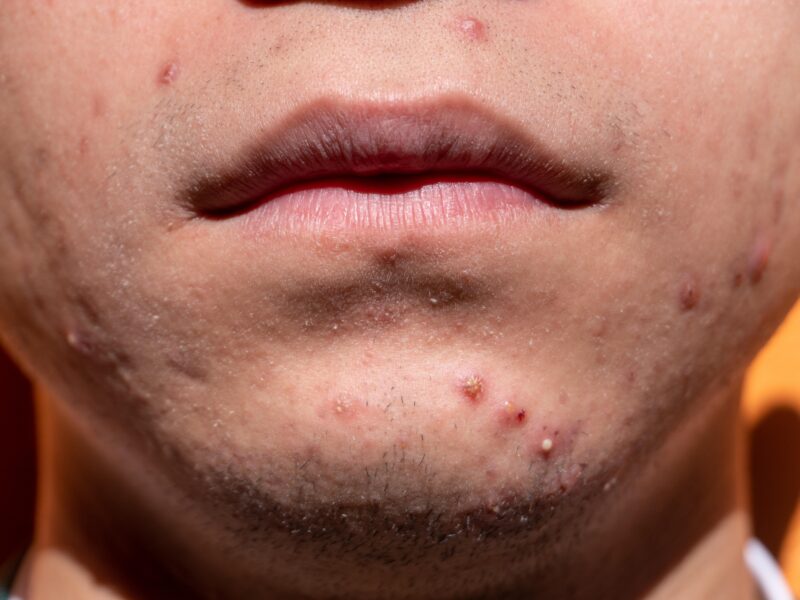
Understanding how a pimple develops explains why each step in your routine exists. Acne forms through a four-stage process.
Stage 1: Excess Sebum Production
Sebaceous glands attached to your hair follicles produce sebum, an oily substance that moisturizes your skin. Hormones (especially androgens like testosterone and DHT) signal these glands to produce more sebum than your skin needs. Excess sebum pools inside the follicle.
Where your routine intervenes: Gentle cleansing removes excess surface sebum without stripping the skin. Harsh cleansers trigger rebound oil production, making the problem worse.
Stage 2: Dead Skin Cell Buildup
Your skin sheds about 30,000 to 40,000 dead cells per hour. In acne-prone skin, these dead cells do not shed normally. They stick together and accumulate inside the pore opening, forming a plug. This plug is a comedone. An open comedone is a blackhead. A closed comedone is a whitehead.
Where your routine intervenes: Retinoids increase cell turnover, preventing dead cells from accumulating and forming plugs. Retinoids are the most effective ingredient for keeping pores clear.
Stage 3: Bacterial Overgrowth
Cutibacterium acnes (C. acnes) is a bacterium living naturally on your skin. When a pore is clogged with sebum and dead cells, C. acnes multiplies inside the oxygen-deprived environment of the blocked follicle. The bacterial population grows rapidly.
Where your routine intervenes: Benzoyl peroxide kills C. acnes bacteria on contact. Unlike topical antibiotics, C. acnes does not develop resistance to benzoyl peroxide. This makes benzoyl peroxide effective for long-term use.
Stage 4: Inflammation
Your immune system detects the bacterial overgrowth and sends white blood cells to the area. This immune response causes redness, swelling, and pain. The result is an inflamed pimple, pustule, or cyst. The more aggressive the immune response, the larger and more painful the lesion.
Where your routine intervenes: Moisturizer and sunscreen protect your skin barrier. A strong barrier reduces overall skin inflammation and speeds healing. Picking or squeezing lesions intensifies the immune response and increases scarring risk.
Every step in the routine below targets one or more of these four stages. That is why the system works when individual products fail.
Your Skin Barrier: Why Protecting It Clears Acne Faster
Your skin barrier is the outermost layer of your epidermis (the stratum corneum). Think of it as a wall of skin cells held together by lipids (fats). This wall keeps moisture in and irritants out.
When your barrier is damaged, moisture escapes. Irritants enter. Your skin becomes dry, red, and sensitized. A damaged barrier triggers an inflammatory cascade that worsens existing acne and creates new breakouts.
Common acne treatments damage the barrier. Benzoyl peroxide dries the skin. Retinoids increase cell turnover and temporarily thin the outer layer. Salicylic acid dissolves the lipids holding your barrier together. Overwashing strips natural oils.
Without barrier repair (moisturizer), these treatments create a cycle: you treat acne, damage the barrier, trigger more inflammation, and produce more acne. The breakout returns. You use more product. The barrier takes more damage. The cycle repeats.
A 2018 study in the Journal of the European Academy of Dermatology and Venereology found that patients using acne medications alongside a barrier-repair moisturizer experienced 30% less irritation and 25% faster clearing compared to patients using the same medications without moisturizer.
Moisturizer is not optional in an acne routine. Moisturizer is essential to making your active ingredients work without causing collateral damage.
Morning Routine: Step by Step
Your morning routine focuses on three goals: clean skin, antibacterial treatment, and sun protection. Four steps. Five minutes total.
Step 1: Cleanse
Wash your face with a gentle, fragrance-free cleanser. Use lukewarm water (not hot). Hot water strips natural lipids and weakens your barrier.
Look for cleansers with a pH between 4.5 and 5.5. This matches the natural pH of your skin. Cleansers with higher pH levels disrupt your acid mantle and increase transepidermal water loss (moisture escaping through the skin).
Avoid cleansers containing sodium lauryl sulfate (SLS). SLS is an aggressive surfactant that strips the skin and triggers irritation in acne-prone skin. Sodium laureth sulfate (SLES) and cocamidopropyl betaine are gentler alternatives.
Pat your face dry with a clean towel. Do not rub. Rubbing creates friction that irritates inflamed lesions.
Step 2: Apply Benzoyl Peroxide
Apply a thin layer of 2.5% benzoyl peroxide gel or cream to acne-prone areas. Focus on the forehead, nose, chin, and cheeks where breakouts appear. A thin layer is enough. More product does not work faster. More product causes more irritation.
Wait 1 to 2 minutes for the benzoyl peroxide to absorb before moving to the next step.
Step 3: Moisturize
Apply a non-comedogenic, oil-free moisturizer to your entire face. This locks in hydration and creates a protective layer between your skin and environmental irritants. The moisturizer also buffers the drying effect of benzoyl peroxide throughout the day.
Look for moisturizers containing ceramides, hyaluronic acid, or niacinamide. Ceramides rebuild the lipid barrier. Hyaluronic acid draws water into the skin. Niacinamide reduces redness and regulates sebum production. A 2019 study in the Journal of Drugs in Dermatology found niacinamide reduced sebum production by 23% after 4 weeks of daily use.
Step 4: Sunscreen
Apply broad-spectrum SPF 30 or higher as the final step. Use about a nickel-sized amount for your face. Spread evenly over all exposed areas including your forehead, nose, ears, and jawline.
Sunscreen is not optional in an acne routine. Benzoyl peroxide and retinoids increase photosensitivity. Without sunscreen, sun exposure causes post-inflammatory hyperpigmentation (dark spots left behind after a pimple heals). These dark spots often last longer than the pimple itself.
Reapply sunscreen every 2 hours if you spend extended time in direct sunlight.
Night Routine: Step by Step
Your night routine focuses on deep cleansing, cell turnover, and overnight repair. Three steps. Five minutes total.
Step 1: Cleanse
Wash your face with the same gentle cleanser you use in the morning. Your evening cleanse removes sunscreen, makeup, dirt, pollution particles, and sebum accumulated throughout the day.
If you wear heavy makeup or waterproof sunscreen, double cleanse. Start with a micellar water or oil-based cleanser to dissolve makeup and sunscreen. Follow with your regular gentle cleanser to remove residue. Two light cleanses are gentler on your barrier than one aggressive scrub.
Step 2: Apply Retinoid
Wait until your skin is completely dry. Applying retinoid to damp skin increases absorption and irritation. Wait 5 to 10 minutes after washing if your skin is sensitive.
Apply a pea-sized amount of retinoid to your entire face. Spread evenly. Avoid the corners of your eyes, nostrils, and lips. These areas have thinner skin and are more susceptible to irritation.
Start with a low-strength retinoid. Adapalene 0.1% (available over the counter in many countries) is a good starting point for most people. Use your retinoid every other night for the first 2 to 4 weeks. Increase to every night once your skin tolerates the product without excessive dryness, peeling, or redness.
Step 3: Moisturize
Wait 5 to 10 minutes after applying retinoid. Then apply your moisturizer. The waiting period allows the retinoid to penetrate the skin before the moisturizer creates a barrier on top.
If you experience significant dryness or peeling during the first few weeks of retinoid use, apply moisturizer first and retinoid on top (“buffering”). This reduces irritation while your skin adjusts. As tolerance builds, switch to applying retinoid directly on clean skin.
Your nighttime moisturizer holds in the retinoid and prevents transepidermal water loss while you sleep. Your skin repairs and regenerates most actively between 11 PM and 4 AM. Moisturizer supports this repair process.
Benzoyl Peroxide: How It Works and How to Use It Safely
Benzoyl peroxide is one of the most studied and effective over-the-counter acne ingredients. It works through a simple mechanism: benzoyl peroxide releases oxygen into the clogged pore. C. acnes bacteria are anaerobic, meaning they thrive without oxygen. The oxygen environment created by benzoyl peroxide kills the bacteria on contact.
Unlike topical antibiotics (clindamycin, erythromycin), C. acnes bacteria do not develop resistance to benzoyl peroxide. A 2019 review in the Journal of the American Academy of Dermatology confirmed this makes benzoyl peroxide suitable for long-term daily use without diminishing effectiveness.
Choosing the Right Strength
Benzoyl peroxide comes in 2.5%, 5%, and 10% concentrations. Research shows all three concentrations kill the same amount of bacteria. A 1986 study in the Journal of the American Academy of Dermatology (still referenced in current guidelines) found 2.5% benzoyl peroxide was equally effective as 10% at reducing acne lesions. The only difference: 10% caused significantly more dryness, peeling, and irritation.
Start with 2.5%. This gives you maximum bacterial kill with minimum barrier damage. Increase to 5% only if 2.5% produces no improvement after 6 to 8 weeks.
Application Tips
- Apply a thin, even layer. A thick layer does not work faster. A thick layer wastes product and increases irritation.
- Apply to the entire acne-prone zone, not individual pimples. Benzoyl peroxide works preventively by killing bacteria before new pimples form.
- Be aware that benzoyl peroxide bleaches fabric. Use white pillowcases and towels. Let the product dry fully before contact with clothing.
- If your skin burns or stings severely after application, your barrier is too compromised. Stop benzoyl peroxide for 3 to 5 days. Focus on moisturizer only. Resume when sensitivity subsides.
Short-Contact Therapy
If full-day wear causes too much dryness, try short-contact therapy. Apply benzoyl peroxide to your skin. Leave the product on for 5 to 10 minutes. Rinse off with lukewarm water. Then continue with moisturizer and sunscreen. A 2010 study in the Journal of Drugs in Dermatology found short-contact benzoyl peroxide produced similar bacterial reduction with 50% less skin irritation compared to leave-on application.
Retinoids: How They Work and How to Start Without Wrecking Your Skin
Retinoids are vitamin A derivatives. They are the single most effective topical ingredient for acne. Dermatologists consider them the backbone of any acne routine.
Retinoids work at the cellular level. They bind to receptors on skin cells and alter gene expression. This produces three effects relevant to acne:
- Increased cell turnover: Dead skin cells shed faster instead of accumulating inside pores. This prevents comedone formation (the Stage 2 trigger described above).
- Normalized keratinization: Retinoids change the way cells lining the pore wall develop, making them less “sticky.” Cells separate and exit the pore normally instead of clumping together to form plugs.
- Anti-inflammatory effects: Retinoids reduce the production of inflammatory mediators in the skin. This decreases the redness and swelling associated with inflamed pimples.
A 2019 Cochrane review analyzing over 30 randomized controlled trials confirmed adapalene and tretinoin (the two most common topical retinoids) significantly reduce both inflammatory and non-inflammatory acne lesions compared to placebo.
Starting a Retinoid Without the Irritation
Retinoids are effective. They are also irritating during the first 2 to 6 weeks of use. This adjustment period (sometimes called “retinization”) includes dryness, flaking, redness, and increased sensitivity. Most people who quit retinoids do so during this phase. Knowing what to expect and how to minimize irritation keeps you on track.
- Start low: Use adapalene 0.1% or tretinoin 0.025%. These are the lowest available concentrations. They produce the same long-term results as higher strengths with less initial irritation.
- Start slow: Apply every third night for the first two weeks. Move to every other night for weeks 3 and 4. Move to nightly use starting week 5 or 6 if your skin tolerates the product without excessive peeling or redness.
- Buffer if needed: Apply moisturizer first. Wait 10 minutes. Apply retinoid on top of the moisturizer. This “buffer” technique reduces the amount of retinoid penetrating the skin at once, lowering irritation. As your skin adjusts over 4 to 6 weeks, switch to applying retinoid on bare skin before moisturizer.
- Use a pea-sized amount: Squeeze a pea-sized dot onto your fingertip. Dot small amounts on your forehead, each cheek, nose, and chin. Spread into a thin, even layer. More product does not speed up results. More product accelerates irritation.
- Avoid sensitive areas: Skip the corners of your nose, the skin directly around your eyes, and your lip line. These areas have thinner skin and react faster to retinoids.
The Retinoid Timeline
- Weeks 1 to 3: Dryness, mild peeling, and possible purging (existing clogged pores surfacing faster). This is normal.
- Weeks 4 to 6: Skin begins adapting. Dryness decreases. New breakouts slow down.
- Weeks 8 to 12: Visible clearing. Pores appear smaller. Skin texture smooths out. Post-inflammatory marks begin fading.
- Months 3 to 6: Full results. Significant reduction in active breakouts and improved overall skin tone.
Retinoids reward patience. The first month is the hardest. The results after month 2 are worth the adjustment period.
Moisturizer for Acne-Prone Skin: Why You Need It and What to Look For
The biggest mistake people with acne make is skipping moisturizer. The logic seems sound: oily skin causes acne, so removing moisture should help. This reasoning is wrong.
Your skin produces oil (sebum) and retains water (hydration). These are two different processes. Sebum comes from sebaceous glands. Hydration comes from the water content in your skin cells and the barrier holding that water in.
When you strip your skin with harsh cleansers or drying treatments without moisturizing, your barrier weakens. Water escapes. Your skin detects the dehydration and responds by producing more sebum to compensate. You end up with skin that is simultaneously dry and oily. Breakouts increase.
A 2014 study in the Journal of Clinical and Aesthetic Dermatology found that patients using a barrier-repair moisturizer alongside benzoyl peroxide tolerated higher concentrations of benzoyl peroxide, experienced fewer side effects, and cleared faster than patients using benzoyl peroxide alone.
Ingredients to Look For
- Ceramides: Lipids that rebuild the structural integrity of your skin barrier. Studies show topical ceramides restore barrier function within 2 to 4 weeks of daily use.
- Hyaluronic acid: A humectant drawing water from the environment into your skin. One molecule of hyaluronic acid holds up to 1,000 times its weight in water. This ingredient hydrates without adding oil or heaviness.
- Niacinamide (Vitamin B3): Reduces redness, regulates sebum production, and strengthens the barrier. A 2006 study in the International Journal of Dermatology found 4% niacinamide gel reduced acne lesions as effectively as 1% clindamycin (a topical antibiotic) over 8 weeks.
- Glycerin: A humectant pulling water into the outer layers of skin. Glycerin is one of the best-studied moisturizing agents with a strong safety profile for sensitive and acne-prone skin types.
Ingredients to Avoid
- Heavy oils: Coconut oil, cocoa butter, and wheat germ oil are comedogenic (pore-clogging) for most acne-prone skin types. Avoid moisturizers listing these as primary ingredients.
- Fragrance: Synthetic fragrances are a leading cause of contact irritation. Irritated skin inflames more easily, worsening acne. Choose fragrance-free formulas. “Unscented” is not the same as “fragrance-free.” Unscented products sometimes contain masking fragrances.
- Isopropyl myristate: A common emollient in cosmetics rated highly comedogenic. Check ingredient labels if you break out from moisturizers despite choosing “oil-free” formulas.
Sunscreen and Acne: Finding the Right Formula
Sunscreen protects healing skin from UV damage. UV exposure worsens post-inflammatory hyperpigmentation (the dark marks left after pimples heal). Without sunscreen, these marks persist for months. With daily sunscreen, they fade significantly within 4 to 8 weeks.
Both benzoyl peroxide and retinoids increase your skin’s sensitivity to UV radiation. Using these products without sunscreen increases your risk of sunburn, hyperpigmentation, and premature aging.
Mineral vs. Chemical Sunscreen for Acne
Mineral sunscreens contain zinc oxide or titanium dioxide. They sit on top of the skin and reflect UV rays. Zinc oxide has mild anti-inflammatory and antimicrobial properties. Mineral sunscreens are less likely to irritate sensitive or inflamed acne-prone skin. The downside: some mineral sunscreens leave a white cast and feel heavier on the skin.
Chemical sunscreens absorb UV rays and convert them to heat. Common active ingredients include avobenzone, octinoxate, and oxybenzone. Chemical sunscreens tend to feel lighter and blend invisibly. Some chemical filters (particularly oxybenzone) cause contact irritation in sensitive skin.
For acne-prone skin, mineral sunscreens with zinc oxide are the safest choice. If you prefer the texture of chemical sunscreens, choose formulas labeled non-comedogenic and oil-free. Avoid any sunscreen that leaves a greasy residue.
Application Tips
- Apply sunscreen as the last step of your morning routine, after moisturizer.
- Use about a nickel-sized amount for your face alone.
- Wait 2 to 3 minutes for the sunscreen to set before applying makeup.
- Reapply every 2 hours during prolonged sun exposure. If you work indoors and are not near windows, morning application is sufficient.
- If your sunscreen causes breakouts, switch to a different formula before stopping sun protection entirely. The right sunscreen for your skin exists. Testing 2 to 3 products is normal.
8 Habits That Prevent Breakouts
Your routine handles cleansing and treatment. These daily habits eliminate the external triggers that cause breakouts between applications.
-
Stop Touching Your Face
Your hands carry bacteria, dirt, and oil from every surface you touch throughout the day. A 2015 study in the American Journal of Infection Control found the average person touches their face 23 times per hour. Each touch transfers bacteria and debris to your skin. If you rest your chin on your hand during desk work, breakouts along your jawline follow. Become aware of the habit. Keep your hands below your chin.
-
Change Your Pillowcase Every 2 to 3 Days
Your pillowcase collects sebum, dead skin cells, bacteria, and product residue every night. Sleeping on a dirty pillowcase reintroduces these pore-clogging substances to your skin for 6 to 8 hours. Rotate to a fresh pillowcase every 2 to 3 days. Flip your pillow to the clean side on alternate nights to extend each pillowcase.
-
Clean Your Phone Screen Daily
Your phone screen presses against your cheek and jawline during calls. A 2012 study at the University of Arizona found cell phones carry 10 times more bacteria than a toilet seat. Wipe your phone screen with an antibacterial wipe or a microfiber cloth dampened with rubbing alcohol once daily. Use speakerphone or earbuds to keep your phone away from your face.
-
Wash Makeup Brushes Weekly
Makeup brushes and sponges accumulate bacteria, oil, and old product with each use. The American Academy of Dermatology recommends cleaning brushes every 7 to 10 days. Use a gentle soap or brush cleanser. Rinse thoroughly. Lay brushes flat to dry. Replace makeup sponges every 1 to 3 months regardless of cleaning frequency.
-
Keep Hair Products Off Your Face
Hair oils, styling products, serums, and dry shampoos contain ingredients that clog pores along your hairline and forehead. This type of acne is called acne cosmetica or pomade acne. If you experience consistent breakouts along your hairline, switch to non-comedogenic hair products and tie your hair back while sleeping.
-
Shower After Sweating
Sweat itself does not cause acne. But sweat sitting on your skin mixes with sebum and bacteria. This mixture clogs pores, especially on your back, chest, and forehead. Shower or wash your face within 30 minutes of finishing a workout. If you are unable to shower immediately, wipe your face and body with a clean towel or micellar water wipe.
-
Manage Stress Actively
Stress increases cortisol production. Cortisol stimulates sebaceous glands to produce more oil. A 2017 study in Clinical, Cosmetic and Investigational Dermatology confirmed a direct correlation between perceived stress levels and acne severity in adult women. The higher the stress score, the worse the breakouts. Exercise, deep breathing, adequate sleep, and time away from screens lower cortisol levels and reduce stress-triggered flares.
-
Sleep 7 to 8 Hours Nightly
Sleep deprivation increases cortisol levels, weakens immune function, and slows skin repair. Your skin does the majority of its cellular repair between 10 PM and 2 AM. Consistent sleep under 6 hours disrupts this repair window. A 2015 study in the journal Sleep found participants sleeping fewer than 5 hours per night showed impaired skin barrier recovery and higher levels of transepidermal water loss compared to participants sleeping 7 to 8 hours.
7 Mistakes That Make Acne Worse
Many common “acne-fighting” habits damage your skin and increase breakouts. Avoid these.
-
Overwashing Your Face
Washing more than twice daily strips your barrier. Your sebaceous glands respond by producing more oil to replace what you removed. The result is oilier, more breakout-prone skin. Wash once in the morning and once at night. That is enough. If your face feels oily at midday, blot with an oil-absorbing sheet instead of washing again.
-
Using Physical Scrubs on Active Breakouts
Scrubs with beads, walnut shells, or rough textures tear at inflamed pimples. This spreads bacteria across your skin, ruptures lesions beneath the surface, and increases scarring risk. Avoid physical exfoliation on active acne. If you want exfoliation, use a chemical exfoliant (salicylic acid or glycolic acid) at low concentrations instead.
-
Picking or Squeezing Pimples
Squeezing forces bacteria and pus deeper into the skin. This creates larger, more inflamed lesions and increases the risk of permanent scarring and post-inflammatory hyperpigmentation. Apply a hydrocolloid pimple patch or benzoyl peroxide spot treatment instead. If a pimple is large and painful, a dermatologist performs a cortisone injection that flattens the lesion within 24 to 48 hours without the tissue damage caused by squeezing.
-
Layering Too Many Active Ingredients
Using benzoyl peroxide, salicylic acid, glycolic acid, and a retinoid at the same time overwhelms your barrier. The cumulative drying and irritating effects trigger more inflammation than the ingredients resolve. Use one active in the morning (benzoyl peroxide). Use one active at night (retinoid). That is enough. Adding more actives increases irritation without increasing efficacy.
-
Changing Products Too Frequently
Skin cell turnover takes about 28 days. You need at least two full cycles (8 weeks) to evaluate whether a product is working. Switching products every 1 to 2 weeks does not give any product enough time to produce results. You also lose track of what caused improvement or worsening. Pick your routine. Stick with the routine for a minimum of 8 weeks before making changes.
-
Skipping Sunscreen Because It “Feels Heavy”
UV exposure without sunscreen worsens hyperpigmentation, increases photosensitivity from acne medications, and accelerates collagen breakdown. If your current sunscreen feels heavy or causes breakouts, switch to a lighter, non-comedogenic formula. Do not stop wearing sunscreen. The right product exists. Finding the right product for your skin takes trial and error.
-
Using Toothpaste, Lemon Juice, or DIY Treatments
Toothpaste contains sodium lauryl sulfate, triclosan, and menthol. These ingredients burn and irritate broken skin. Lemon juice has a pH of 2, far below your skin’s natural pH of 4.5 to 5.5. Applying it causes chemical burns and increases sun sensitivity. DIY treatments are unpredictable, unstandardized, and frequently damaging. Use products formulated and tested for facial skin.
Purging vs. Breakouts: How to Tell the Difference
When you start a retinoid, your skin pushes existing clogged pores to the surface faster than normal. This is called purging. Purging looks like a breakout but follows specific patterns.
Signs of Purging
- Breakouts appear in areas where you normally get pimples.
- Pimples are small, come to a head quickly, and heal faster than your usual breakouts.
- The number of new lesions decreases week by week.
- Purging resolves within 4 to 6 weeks of starting the new product.
Signs of a Reaction (Not Purging)
- Breakouts appear in areas where you do not normally get pimples.
- Lesions are deep, inflamed, and painful.
- Redness and irritation spread across your entire face, not limited to breakout zones.
- Breakouts worsen over 6 weeks or more without improvement.
If your skin is purging, continue the retinoid. The breakout is temporary. Existing clogs are surfacing and clearing. If your skin is reacting, stop the product. Return to gentle cleansing and moisturizer only for 2 weeks. Then reintroduce products one at a time to identify the trigger.
Does Diet Affect Acne?
Research on diet and acne has increased significantly over the past decade. The evidence points to two dietary factors with the strongest connection to breakout severity.
High-Glycemic Foods
Foods that spike blood sugar rapidly (white bread, sugary drinks, white rice, pastries, candy) increase insulin levels. Elevated insulin stimulates androgen production and increases sebum output. A 2007 study in the American Journal of Clinical Nutrition followed 43 males with acne for 12 weeks. The group eating a low-glycemic diet experienced a 22% reduction in acne lesions compared to the control group eating a standard diet.
A 2020 review in the Journal of the American Academy of Dermatology confirmed the association between high-glycemic diets and increased acne severity across multiple studies.
Dairy
Skim milk shows the strongest association with acne among dairy products. Researchers believe this connection relates to the hormones and bioactive molecules naturally present in cow’s milk. A 2018 meta-analysis in Nutrients analyzed 14 studies involving over 78,000 participants. The analysis found dairy consumption (especially skim milk) was associated with a 25% increased risk of acne.
Whole milk showed a weaker association than skim milk. Yogurt and cheese showed the weakest associations. The relationship between dairy and acne varies by individual.
What to Do About Diet and Acne
You do not need to eliminate food groups. But paying attention to patterns helps. Keep a simple food diary for 4 weeks. Note what you eat daily alongside your skin’s condition. If you notice breakouts consistently worsening 24 to 48 hours after specific foods, reduce those foods and observe whether your skin improves.
Prioritize whole foods, vegetables, fruits, lean proteins, and water. These foods provide lower glycemic loads and support overall skin health. Diet works alongside your topical routine, not as a replacement for the routine itself.
When to See a Dermatologist
Home routines work for mild to moderate acne. Some forms of acne need professional treatment. See a dermatologist if you experience any of the following.
- Deep, painful cysts or nodules: These form deep beneath the skin surface. Topical products do not penetrate deeply enough to treat them. Dermatologists treat cystic acne with prescription oral medications (isotretinoin, spironolactone, antibiotics), cortisone injections, and professional-grade topical retinoids.
- Scarring: If your acne leaves indented (atrophic) or raised (hypertrophic) scars, early intervention prevents permanent damage. Dermatologists offer treatments including chemical peels, microneedling, laser resurfacing, and dermal fillers to address scarring.
- No improvement after 8 to 12 weeks of consistent home care: If you follow the routine in this guide daily for 3 months and see no improvement, your acne requires prescription-strength treatment. A dermatologist assesses your specific acne type and tailors a treatment plan.
- Acne affecting your mental health: Acne impacts self-esteem, social confidence, and daily quality of life. A 2018 study in the British Journal of Dermatology found that acne patients have a 63% higher risk of developing depression compared to those without acne. If breakouts affect how you feel about yourself or limit your willingness to participate in daily activities, seek professional help. Faster clearing is available.
- Acne appearing suddenly in adulthood: New-onset acne after age 25, especially along the jawline and chin in women, often signals hormonal changes. Polycystic ovary syndrome (PCOS), thyroid conditions, and other hormonal imbalances cause adult acne that does not respond to standard topical treatment alone. A dermatologist or endocrinologist identifies the hormonal driver and treats the root cause.
- Signs of infection: Increasing redness spreading beyond the pimple, warmth, pus, swelling, or fever indicate a possible skin infection requiring antibiotics. See a doctor promptly if these signs develop.
Your Weekly Schedule at a Glance
Use this schedule as a reference during your first 6 weeks. Adjust retinoid frequency based on your skin’s tolerance.
| Time of Day | Step | Product | Frequency |
|---|---|---|---|
| Morning | Cleanse | Gentle, fragrance-free cleanser | Every day |
| Morning | Treat | Benzoyl peroxide 2.5% | Every day |
| Morning | Moisturize | Non-comedogenic moisturizer | Every day |
| Morning | Protect | Broad-spectrum SPF 30+ | Every day |
| Night | Cleanse | Gentle, fragrance-free cleanser | Every day |
| Night | Treat | Retinoid (adapalene 0.1%) | Weeks 1 to 2: every 3rd night. Weeks 3 to 4: every other night. Week 5 onward: every night. |
| Night | Moisturize | Non-comedogenic moisturizer | Every day |
This schedule gives you 4 morning products and 3 nighttime products. Total products in your routine: 5 (cleanser, benzoyl peroxide, moisturizer, sunscreen, retinoid). Keep the routine simple. Fewer products mean less risk of irritation, lower cost, and higher consistency.
Start Tonight
Acne responds to systems. Not individual products. Not sporadic effort. Not complicated 12-step routines.
Your system is simple. Cleanse gently. Treat with benzoyl peroxide in the morning and a retinoid at night. Moisturize after every treatment. Wear sunscreen every morning. Protect your barrier.
The first 2 to 4 weeks test your patience. Your skin adjusts. Purging happens. Dryness shows up. This is the adjustment period. Push through the adjustment phase with consistent application and adequate moisturizer.
By week 6, new breakouts slow down. By week 8 to 12, your skin looks noticeably clearer. By month 3 to 6, the full results of your routine become visible.
Start tonight. Wash your face with a gentle cleanser. Apply moisturizer. That is step one. Add benzoyl peroxide tomorrow morning. Add your retinoid later this week. Build the routine piece by piece. Your skin adapts better when you introduce products gradually.
Be patient. Be consistent. Your skin replaces itself every 28 days. Give the routine time to work. The results will follow.
Frequently Asked Questions
How long does an acne routine take to show results?
Most people notice fewer new breakouts within 4 to 6 weeks of consistent daily use. Visible clearing takes 8 to 12 weeks. Skin cells turn over in approximately 28-day cycles. Give any new routine at least two full turnover cycles before evaluating results. Changing products before the 8-week mark does not give your skin enough time to respond.
Should I use benzoyl peroxide and retinoids at the same time?
Not at the same time of day. Benzoyl peroxide degrades certain retinoids (especially tretinoin) on contact, reducing their effectiveness. Use benzoyl peroxide in the morning and your retinoid at night. This separation gives you the antibacterial benefits of benzoyl peroxide during the day and the pore-clearing benefits of your retinoid overnight. Adapalene is more stable with benzoyl peroxide than tretinoin, but separating them by time of day is still the safest approach.
Do I need moisturizer if my skin is oily?
Yes. Oily skin still needs hydration. Oil production and hydration are two separate processes. Skipping moisturizer weakens your barrier. A weakened barrier signals your sebaceous glands to produce more oil as a protective response. You end up oilier. Use a lightweight, non-comedogenic, oil-free moisturizer. Your skin stays hydrated without added shine or pore congestion. Gel-based moisturizers work well for oily skin types.
What does non-comedogenic mean?
Non-comedogenic means the product is formulated to not block pores. Comedones are clogged pores (blackheads and whiteheads). Products labeled non-comedogenic have been tested to confirm they do not increase pore blockage. Look for this label on every moisturizer, sunscreen, and makeup product you apply to acne-prone areas. The label does not guarantee zero breakouts for every person, but the risk is significantly lower than with non-labeled products.
Is it okay to pop a pimple at home?
No. Squeezing or popping pimples pushes bacteria and inflammation deeper into the skin. This increases the risk of scarring, hyperpigmentation, and secondary infection. Apply a hydrocolloid pimple patch to draw out fluid overnight. Or apply benzoyl peroxide as a spot treatment. If a pimple is large and painful, a dermatologist performs a safe cortisone injection that flattens the lesion within 24 to 48 hours without tissue damage.
Does diet affect acne?
Research supports a connection for some people. A 2020 review in the Journal of the American Academy of Dermatology found high-glycemic diets (white bread, sugary drinks, processed snacks) and dairy consumption (especially skim milk) are associated with increased acne severity. Dietary triggers vary by individual. Keeping a food diary for 4 weeks helps identify your personal patterns. Diet works alongside your topical routine. Diet does not replace your topical routine.
When should I see a dermatologist for acne?
See a dermatologist if your acne includes deep, painful cysts that do not respond to over-the-counter products. If your routine has not improved your skin after 8 to 12 weeks of consistent daily use. If you are developing scars. If acne affects your mental health or daily confidence. Prescription treatments like topical antibiotics, oral medications, and professional-grade retinoids address acne that home routines alone do not resolve.
Does sunscreen make acne worse?
The wrong sunscreen does. Heavy, oil-based sunscreens clog pores and trigger breakouts. Look for sunscreens labeled non-comedogenic, oil-free, and lightweight. Mineral sunscreens containing zinc oxide or titanium dioxide sit on top of the skin rather than absorbing into pores. Zinc oxide also provides mild anti-inflammatory properties beneficial for acne-prone skin. Testing 2 to 3 sunscreens to find your best formula is normal.
What is purging and how do I tell the difference from a breakout?
Purging happens when a cell-turnover product (retinoid, chemical exfoliant) brings existing clogged pores to the surface faster than normal. Purging appears in areas where you normally break out and resolves within 4 to 6 weeks. Pimples during purging tend to be smaller and heal faster. A reaction breakout appears in new areas, includes widespread redness and irritation, and worsens over time without improvement. If breakouts appear in unusual areas after starting a new product, stop using the product.
How do I know if my skin barrier is damaged?
A damaged barrier shows specific signs: stinging when you apply products that previously caused no sensation, persistent tightness and dryness even after moisturizing, unusual redness and sensitivity, and flaking that does not improve with hydration. If your skin stings when you apply moisturizer or water, your barrier needs repair. Stop all active ingredients (benzoyl peroxide, retinoids, exfoliants). Use only a gentle cleanser and a ceramide-rich moisturizer for 1 to 2 weeks until sensitivity resolves. Then reintroduce active ingredients one at a time at reduced frequency.