Natural remedies for rheumatoid arthritis pain offer genuine relief when you feel like your own body has turned against you, and the morning stiffness makes even simple tasks feel impossible. If you are living with rheumatoid arthritis, you already know that managing pain goes beyond just taking medication. The constant inflammation, the unpredictable flare ups, and the daily discomfort can drain your energy and test your patience in ways that people without this condition simply cannot understand.
The good news is that science has validated many natural approaches that can work alongside your medical treatment. These are not magical cures or empty promises, but evidence-based strategies that real people use every day to reclaim their quality of life. Think of these remedies as additional tools in your wellness toolkit, each one addressing different aspects of rheumatoid arthritis pain and inflammation.
Understanding Rheumatoid Arthritis Pain
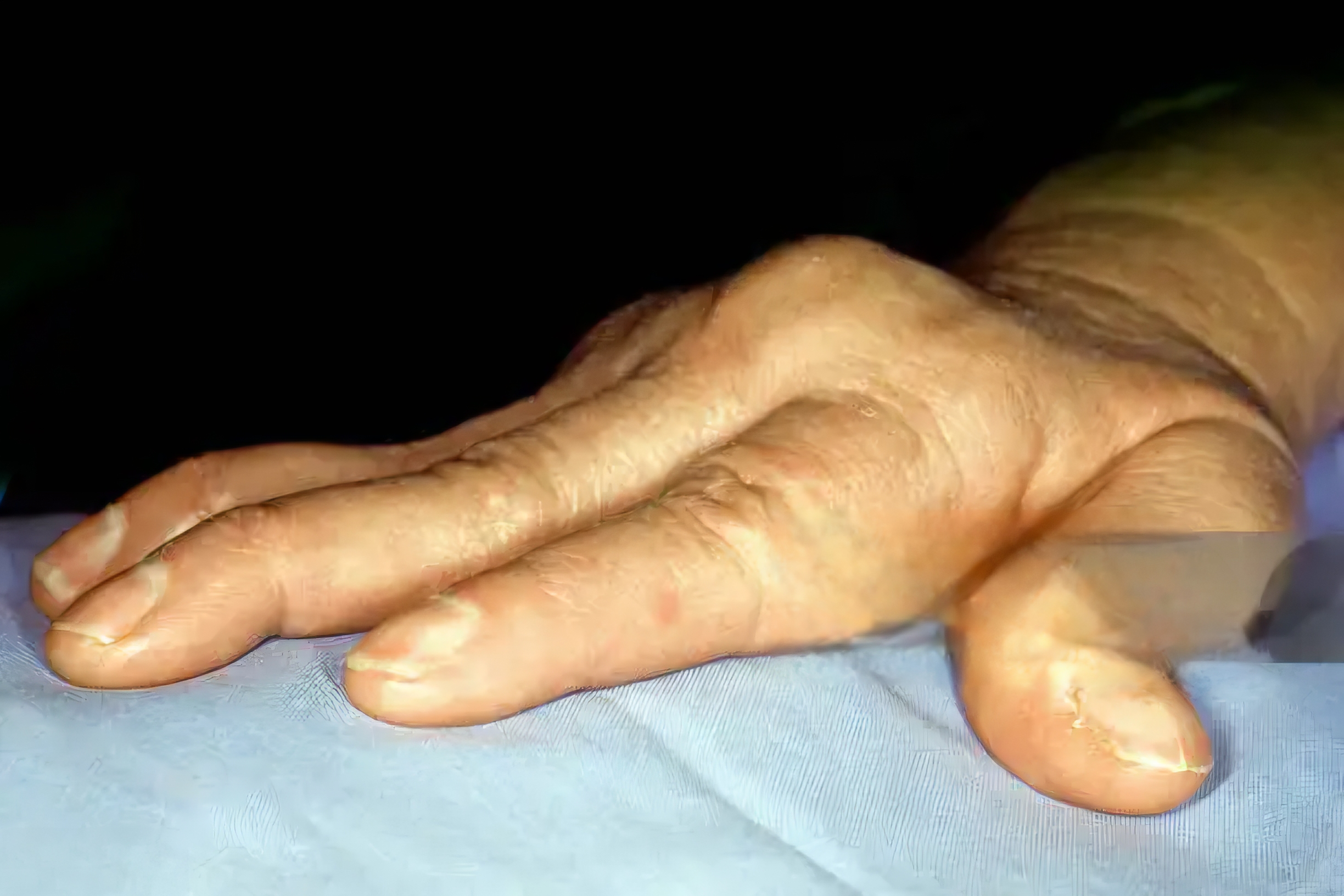
Before diving into solutions, it helps to understand what you are actually dealing with. Rheumatoid arthritis is not just regular wear and tear on your joints. This is an autoimmune condition where your immune system mistakenly attacks the lining of your joints, causing inflammation that leads to pain, swelling, and eventually joint damage if left unchecked.
Unlike osteoarthritis that typically affects one or two joints from overuse, rheumatoid arthritis usually shows up symmetrically. When your right wrist hurts, your left one probably does too. This pattern happens because the immune system is systemically overactive, not because you injured a specific joint. Understanding this distinction matters because it explains why natural remedies that calm inflammation throughout your whole body can be so effective.
Anti-Inflammatory Foods That Actually Make a Difference
Your diet plays a much bigger role in managing rheumatoid arthritis pain than most people realize. Food is not just fuel, it is information that tells your body whether to ramp up inflammation or calm it down. When you eat foods rich in omega-3 fatty acids, antioxidants, and specific plant compounds, you are essentially sending anti-inflammatory signals throughout your system.
Fatty fish like salmon, mackerel, and sardines contain high levels of EPA and DHA, two omega-3 fatty acids that directly reduce the production of inflammatory molecules in your body. Research shows that people who eat fish regularly often experience less morning stiffness and can sometimes reduce their need for anti-inflammatory medications. Aim for at least two servings per week, and if you cannot stand fish, high-quality fish oil supplements offer similar benefits.
Colorful fruits and vegetables are not just pretty on your plate. The pigments that give blueberries their deep blue color, tomatoes their red hue, and leafy greens their vibrant color are actually powerful antioxidants called phytonutrients. These compounds neutralize free radicals that contribute to inflammation and tissue damage. Berries, cherries, spinach, kale, and sweet potatoes should become regular features in your meals, not occasional guests.
Turmeric deserves special attention because its active compound, curcumin, has been studied extensively for arthritis. This golden spice blocks inflammatory pathways at the molecular level, similar to how some medications work but without the side effects. However, curcumin absorbs poorly on its own, so always combine it with black pepper, which increases absorption by up to 2000%. You can add turmeric to smoothies, curries, soups, or take it as a supplement standardized to contain 95% curcuminoids.
Extra virgin olive oil contains oleocanthal, a natural compound that works similarly to ibuprofen by inhibiting inflammatory enzymes. Using olive oil as your primary cooking fat and drizzling it generously over salads and vegetables gives you a daily dose of anti-inflammatory protection. Just make sure to buy quality olive oil stored in dark bottles, and never heat it to smoking temperatures which destroys its beneficial compounds.
Foods That Trigger Inflammation
Knowing what to add matters, but knowing what to remove can be equally important. Some foods act like gasoline on the inflammatory fire, and identifying your personal triggers can dramatically reduce pain levels. This process requires some detective work because not everyone reacts to the same foods.
Refined sugars and carbohydrates cause rapid spikes in blood sugar, which triggers inflammatory responses throughout your body. When you eat white bread, pastries, sugary drinks, or candy, you are essentially choosing temporary pleasure over long-term pain relief. Swap these for whole grains, and notice how your energy stabilizes and your joints feel better.
Some people with rheumatoid arthritis find that nightshade vegetables like tomatoes, peppers, eggplants, and potatoes worsen their symptoms. The theory is that solanine, a compound in nightshades, may trigger inflammation in susceptible individuals. This is controversial and not universally true, but if you suspect nightshades bother you, try eliminating them for three weeks and see if you notice improvement.
Processed foods loaded with trans fats, artificial additives, and preservatives can promote inflammation. These foods are designed for shelf stability and profit margins, not for your joint health. Reading ingredient labels becomes crucial. If you cannot pronounce an ingredient or if sugar appears in the first three items, put it back on the shelf.
The Power of Movement and Exercise
When your joints hurt, the last thing you want to do is move them. This instinct to rest and protect painful joints makes sense, but it actually backfires over time. Gentle, appropriate exercise is one of the most effective natural remedies for rheumatoid arthritis pain, and research consistently shows that people who stay active manage their condition better than those who become sedentary.
Exercise reduces inflammation through multiple mechanisms. Physical activity helps regulate your immune system, reduces inflammatory markers in your blood, maintains healthy joint fluid circulation, and prevents the muscle weakness that makes arthritis worse. The key word here is appropriate because high-impact activities can indeed cause more harm than good.
Swimming and water aerobics top the list for rheumatoid arthritis because water supports your body weight, removing stress from your joints while still providing resistance for strength building. The warmth of a heated pool also soothes stiff joints and relaxes tense muscles. Many people who cannot walk for ten minutes on land can exercise for 30 minutes or more in water without pain.
Tai chi, an ancient Chinese practice involving slow, flowing movements and deep breathing, has been specifically studied for arthritis. Multiple research studies show that regular tai chi practice reduces pain, improves balance, and enhances overall physical function in people with rheumatoid arthritis. The meditative aspect also helps manage the stress and anxiety that often accompany chronic pain conditions.
Gentle yoga adapted for arthritis can improve flexibility, strengthen muscles around your joints, and teach you body awareness that helps you move more efficiently throughout the day. Look for classes specifically designed for arthritis or work with an instructor who understands your limitations. Avoid any pose that causes sharp pain, and remember that yoga should never be about forcing your body into uncomfortable positions.
Walking remains one of the simplest yet most effective exercises. Start with just five or ten minutes if that is all you can manage, and gradually build up. Good supportive shoes make an enormous difference. Walk on soft surfaces like grass or tracks rather than concrete when possible, and pay attention to your body’s signals.
Heat and Cold Therapy
Temperature therapy is an ancient remedy that modern science has validated. Both heat and cold reduce pain, but they work through different mechanisms and are useful in different situations. Learning when to use each gives you a simple, free tool you can apply anytime, anywhere.
Heat therapy works by increasing blood flow to the area, which brings oxygen and nutrients while washing away inflammatory waste products. Heat also relaxes muscles and increases tissue flexibility. Use heat for morning stiffness, chronic aching pain, and before exercise to warm up your joints. A warm shower, heating pad, warm paraffin wax treatments, or even warm, moist towels all work well. Apply heat for 15 to 20 minutes at a time.
Cold therapy numbs pain, reduces swelling, and slows down the inflammatory process by constricting blood vessels. Use cold therapy during acute flare ups when joints are hot, red, and swollen, or after activity that might have irritated your joints. Ice packs, frozen vegetables wrapped in a towel, or cold gel packs should be applied for no more than 15 minutes at a time to avoid tissue damage. Always place a barrier like a thin towel between ice and your skin.
Some people benefit from contrast therapy, alternating between hot and cold. This creates a pumping action in your blood vessels that can be particularly effective for reducing swelling. Try three minutes of heat followed by one minute of cold, repeating this cycle three to five times and always ending with cold.
Herbal Remedies Backed by Research
Certain herbs have been used for centuries to treat joint pain, and modern research has identified why they work. While herbs are natural, they are also pharmacologically active, meaning they can interact with medications and have side effects. Always discuss herbal remedies with your healthcare provider before starting them.
Ginger contains compounds called gingerols that block inflammatory pathways and reduce pain. Studies comparing ginger to placebo consistently show that ginger reduces arthritis pain and improves function. You can consume ginger as fresh root grated into food, steeped as tea, or taken as standardized supplements. A typical effective dose is 500 to 1000 mg daily.
Boswellia, also called Indian frankincense, contains boswellic acids that inhibit inflammatory enzymes. Research shows boswellia can reduce pain and improve mobility in people with arthritis. Look for supplements standardized to contain at least 60% boswellic acids, and expect to take it for at least four weeks before seeing full benefits.
Green tea is loaded with polyphenols, particularly epigallocatechin-3-gallate or EGCG, which has powerful anti-inflammatory and antioxidant properties. Laboratory studies show that EGCG can actually slow cartilage destruction. Drinking three to four cups of quality green tea daily provides therapeutic amounts, or you can take EGCG supplements if you prefer.
Willow bark, the original source of aspirin, contains salicin which your body converts to salicylic acid. This provides pain relief and reduces inflammation similar to aspirin but generally with fewer stomach side effects. However, anyone allergic to aspirin should avoid willow bark, and it can still interact with blood thinners.
The Gut Health Connection
This might surprise you, but your gut health directly affects your rheumatoid arthritis. About 70% of your immune system resides in and around your digestive tract, and the balance of bacteria in your gut influences whether your immune system stays calm or becomes overactive.
Research increasingly shows that people with rheumatoid arthritis often have altered gut bacteria compositions compared to healthy individuals. This imbalance, called dysbiosis, can trigger and perpetuate the autoimmune response. Supporting gut health through diet and probiotics may help calm the immune system and reduce inflammation.
Probiotic-rich foods like yogurt with live cultures, kefir, sauerkraut, kimchi, and other fermented vegetables introduce beneficial bacteria into your digestive system. These good bacteria compete with harmful ones, produce anti-inflammatory compounds, and help regulate immune function. Try to include at least one serving of fermented food daily.
Prebiotic foods feed the good bacteria already living in your gut. Foods high in prebiotic fiber include garlic, onions, leeks, asparagus, bananas, and whole grains. Think of probiotics as the seeds and prebiotics as the fertilizer. You need both for a healthy gut garden.
High-quality probiotic supplements can also help, especially strains like Lactobacillus and Bifidobacterium species that have been studied in inflammatory conditions. Look for products with at least several billion colony-forming units and multiple strains. Keep them refrigerated to maintain potency.
Stress Management and Mind-Body Techniques
Stress does not just make you feel bad mentally, it creates real physical inflammation that worsens rheumatoid arthritis. When you are stressed, your body releases cortisol and other stress hormones that, in chronic excess, actually promote inflammation rather than reduce it. Managing stress is not optional self-care, it is essential medicine for your condition.
Meditation and mindfulness practices have been studied extensively for chronic pain. Research shows that regular meditation can reduce pain intensity, improve function, and decrease inflammatory markers in people with arthritis. You do not need to sit in lotus position for hours. Even five or ten minutes daily of focused breathing and present-moment awareness provides benefits.
Deep breathing exercises activate your parasympathetic nervous system, the rest and digest mode that counters stress responses. Try this simple technique several times daily: breathe in slowly for a count of four, hold for four, exhale for six, and pause for two. The longer exhale signals your body to relax. Repeat for five to ten cycles.
Progressive muscle relaxation involves systematically tensing and then releasing different muscle groups throughout your body. This practice not only reduces overall tension but also teaches you to recognize when you are holding stress in your body so you can consciously release it. Many free guided sessions are available online or through apps.
Cognitive behavioral therapy, especially when focused on pain management, teaches you to recognize and change thought patterns that amplify pain perception. Working with a therapist trained in CBT for chronic pain can give you practical tools for managing the psychological burden of rheumatoid arthritis.
Sleep Quality and Pain Management
Poor sleep makes pain worse, and pain makes sleep difficult. This vicious cycle traps many people with rheumatoid arthritis in a pattern of exhaustion and increased suffering. Breaking this cycle by improving sleep quality can significantly reduce your pain levels and improve your ability to cope with your condition.
Sleep is when your body performs most of its repair and recovery work. During deep sleep, growth hormone is released, tissues are rebuilt, and the immune system recalibrates. When you regularly miss out on quality sleep, inflammation increases, pain sensitivity heightens, and your condition becomes harder to manage.
Create a sleep sanctuary by making your bedroom dark, cool, and quiet. Blackout curtains, white noise machines, and keeping the temperature around 65 to 68 degrees Fahrenheit all promote better sleep. Invest in a supportive mattress and pillows that keep your joints in comfortable, neutral positions.
Establish a consistent sleep schedule by going to bed and waking up at the same time every day, even on weekends. Your body thrives on routine, and a regular schedule strengthens your natural circadian rhythm, making it easier to fall asleep and wake refreshed.
Limit screen time for at least an hour before bed. The blue light from phones, tablets, and computers suppresses melatonin production, making it harder to fall asleep. If you must use devices, enable night mode or wear blue-light-blocking glasses in the evening.
Gentle stretching or a warm bath before bed can ease joint stiffness and help you relax into sleep. Adding Epsom salts to your bath provides magnesium, which many people are deficient in and which supports both muscle relaxation and sleep quality.
Supplements That Support Joint Health
While whole foods should form the foundation of your nutrition, certain supplements can fill gaps and provide concentrated doses of beneficial compounds that are hard to obtain through diet alone. Quality matters enormously with supplements, so choose reputable brands that undergo third-party testing.
Omega-3 fatty acids in supplement form allow you to achieve therapeutic doses that would be difficult to get from food alone. Studies on rheumatoid arthritis typically use 2 to 3 grams of combined EPA and DHA daily. Look for molecularly distilled fish oil to ensure purity, or consider algae-based omega-3s if you are vegetarian.
Vitamin D deficiency is common in people with rheumatoid arthritis and low levels are associated with increased disease activity. Vitamin D modulates immune function and has anti-inflammatory properties. Have your levels tested and supplement as needed to maintain optimal ranges, typically between 40 to 60 ng/mL. Most people need 2000 to 4000 IU daily, but some require more.
Glucosamine and chondroitin are building blocks of cartilage and joint fluid. While research shows mixed results, many people report that these supplements reduce pain and improve function, particularly when taken consistently for several months. The typical dose is 1500 mg of glucosamine and 1200 mg of chondroitin daily.
Methylsulfonylmethane, commonly called MSM, provides sulfur that your body uses to maintain healthy connective tissue. Studies suggest MSM reduces pain and improves physical function in people with arthritis. A typical dose ranges from 1500 to 3000 mg daily, split into two or three doses.
Magnesium supports over 300 biochemical reactions in your body, including muscle and nerve function. Many people with chronic pain are deficient in magnesium. Supplementing can reduce muscle tension, improve sleep, and support overall pain management. Magnesium glycinate or citrate are well-absorbed forms, with typical doses of 300 to 400 mg daily.
Acupuncture and Traditional Chinese Medicine
Acupuncture has been used for thousands of years to treat pain, and modern research has validated its effectiveness for various types of arthritis pain. While we still do not fully understand all the mechanisms, acupuncture clearly triggers the release of natural pain-relieving chemicals, improves blood flow, and may modulate immune function.
Multiple studies show that acupuncture can reduce pain and improve function in people with rheumatoid arthritis. The treatment involves inserting very thin needles into specific points on your body. Most people find it surprisingly painless, often describing a mild tingling or dull ache when needles are inserted, followed by deep relaxation during the treatment.
Finding a qualified practitioner matters. Look for someone licensed in acupuncture with specific experience treating arthritis. Many people notice improvement after four to six sessions, though some benefit from ongoing maintenance treatments every few weeks.
Acupressure applies pressure to the same points used in acupuncture but without needles. You can learn to do this yourself, making it a free self-care tool you can use anytime. Several studies show that self-administered acupressure reduces arthritis pain and stiffness when practiced regularly.
Massage Therapy for Pain Relief
Therapeutic massage offers more than temporary relaxation. Regular massage reduces pain, decreases stress hormones, improves circulation, and increases range of motion in affected joints. The key is finding a massage therapist trained in working with arthritis who understands how to adjust pressure and techniques for inflamed joints.
Swedish massage uses long, flowing strokes and gentle kneading that promote relaxation and improve circulation without aggravating sensitive joints. This gentle approach works well during flare ups or when pain levels are high.
Deep tissue massage applies more pressure to reach deeper muscle layers and release chronic tension patterns. This can be helpful between flare ups for addressing muscle tightness that develops around painful joints, but it should be avoided during active inflammation.
Self-massage using your hands or simple tools like massage balls gives you control over pressure and allows you to target specific sore spots daily. Even five or ten minutes of gentle self-massage before bed or after waking can reduce stiffness and improve comfort.
Weight Management and Joint Health
Carrying extra weight puts additional mechanical stress on weight-bearing joints like knees, hips, and ankles. Beyond the mechanical load, fat tissue is not inert. It actively produces inflammatory chemicals called adipokines that circulate throughout your body and can worsen rheumatoid arthritis.
Research shows that even modest weight loss can significantly reduce pain and improve function in people with arthritis. Losing just 10% of your body weight can cut pain levels nearly in half for many people. The challenge is losing weight when pain limits your activity, but it is absolutely possible with the right approach.
Focus on the dietary strategies already discussed rather than extreme calorie restriction, which can backfire by slowing metabolism and increasing stress hormones. An anti-inflammatory diet rich in whole foods naturally supports healthy weight because it emphasizes nutrient-dense, filling foods while eliminating empty calories from processed items.
Combine dietary changes with whatever movement you can manage. Remember that you cannot outrun a bad diet, so prioritize food quality first. As you lose weight and your joints hurt less, you will naturally be able to increase activity, creating a positive cycle of improvement.
Topical Treatments That Work
Applying treatments directly to painful joints allows you to deliver relief exactly where you need it without systemic side effects. Several topical options have good research support and can be used alongside other remedies.
Capsaicin cream, made from hot chili peppers, works by depleting substance P, a chemical that transmits pain signals. It causes a warming or burning sensation initially, but with regular use over several weeks, many people experience significant pain reduction. Apply it three to four times daily, and always wash your hands thoroughly afterward to avoid getting it in your eyes.
Menthol and camphor-based products create a cooling sensation that provides temporary pain relief by stimulating sensory receptors that override pain signals. These work quickly, making them useful for breakthrough pain, though the effect is temporary.
Arnica gel or cream, made from a mountain plant, has anti-inflammatory properties when applied topically. Several studies show that arnica reduces arthritis pain and stiffness. Apply it two to three times daily to affected joints.
Essential oils like lavender, eucalyptus, and frankincense have anti-inflammatory and pain-relieving properties. Dilute essential oils in a carrier oil like coconut or jojoba oil before applying to skin. A typical dilution is 3 to 5 drops of essential oil per teaspoon of carrier oil. Gently massage into painful joints.
Creating Your Personal Relief Plan
With so many natural remedies available, you might feel overwhelmed about where to start. The most effective approach is not trying everything at once, but rather building a personalized plan based on your specific symptoms, lifestyle, and preferences.
Start with the foundation: diet, sleep, and stress management. These three pillars affect everything else and provide the base upon which other remedies work more effectively. Spend a month really dialing in an anti-inflammatory diet, improving your sleep habits, and practicing daily stress reduction before adding more interventions.
Keep a symptom journal to track what helps and what does not. Rate your pain, stiffness, and energy levels daily, and note which remedies you tried, what you ate, how you slept, and your stress levels. Patterns will emerge that help you identify your personal triggers and most effective treatments.
Add one new remedy at a time and give it at least three to four weeks before deciding if it helps. This patience allows you to clearly see what works rather than changing too many variables at once and never knowing what actually made a difference.
Work with your healthcare team rather than going it alone. Share your interest in natural remedies with your rheumatologist and primary care doctor. Most physicians appreciate patients who take an active role in their care and can offer guidance on which approaches are safest and most likely to help your specific situation.
Remember that natural remedies work best as complementary approaches alongside medical treatment, not as replacements. Continue taking prescribed medications unless your doctor advises otherwise. Many people find that using natural remedies allows them to eventually reduce medication doses, but this should only happen under medical supervision.
When to Seek Medical Attention
Natural remedies can do a lot, but they cannot replace proper medical care for rheumatoid arthritis. This is a serious condition that can cause permanent joint damage if not properly managed. Certain situations require immediate professional attention.
Sudden, severe worsening of symptoms, especially if accompanied by fever, could indicate infection or a serious flare that needs medical intervention. Joints that become extremely swollen, hot, and red also warrant prompt evaluation.
If you notice symptoms spreading to new joints or developing systemic symptoms like significant fatigue, weight loss, or shortness of breath, contact your rheumatologist. Rheumatoid arthritis can affect organs beyond joints, and these symptoms might indicate complications.
Any remedy, natural or otherwise, that causes new symptoms like rash, digestive upset, or any concerning reaction should be stopped, and you should consult your healthcare provider. Just because something is natural does not mean it cannot cause side effects or allergic reactions.
Regular monitoring with your rheumatologist remains essential even when you feel well. Blood tests that measure inflammation levels and check for organ involvement help catch problems early before permanent damage occurs.
Final Thoughts
Living with rheumatoid arthritis requires patience, persistence, and a willingness to become an active participant in your own care. Natural remedies offer real benefits that can substantially improve your quality of life, but they work best when viewed as part of a comprehensive approach that includes medical care, lifestyle modifications, and self-compassion.
Some days will be harder than others. You will have setbacks and flares despite your best efforts. That is the nature of this condition, and it does not mean you are failing. Progress with rheumatoid arthritis is rarely linear, but over time, as you find the combination of remedies that work for your unique body, you will likely notice that good days outnumber bad ones.
Pay attention to the small victories. Maybe you can now open a jar that would have been impossible last month. Perhaps you walked a bit further today than you could last week. These incremental improvements add up to meaningful changes in your daily life and independence.
Connect with others who understand what you are going through. Support groups, whether in-person or online, provide emotional support and practical tips that only people living with rheumatoid arthritis truly understand. You are not alone in this journey, and learning from others can help you discover new strategies and feel less isolated.
Above all, remember that you are more than your arthritis. This condition is something you manage, not something that defines you. With the right combination of medical care, natural remedies, and self-care practices, you can live a full, meaningful life despite rheumatoid arthritis.
Disclaimer
The information provided in this article is for educational purposes only and is not intended to replace professional medical advice, diagnosis, or treatment. Rheumatoid arthritis is a serious medical condition that requires proper diagnosis and management by qualified healthcare professionals. Always consult with your physician, rheumatologist, or other qualified healthcare provider before starting any new treatment, supplement, exercise program, or making changes to your existing medical regimen.
Natural remedies can interact with medications, may not be appropriate for all individuals, and can cause side effects. What works for one person may not work for another, and some remedies may be contraindicated based on your specific health conditions, medications, or other factors. Never stop taking prescribed medications without consulting your healthcare provider, as doing so could result in serious health consequences.
If you experience severe symptoms, sudden worsening of your condition, signs of infection, or any concerning reactions to natural remedies, seek immediate medical attention. The authors and publishers of this article are not responsible for any adverse effects or consequences resulting from the use of any suggestions, preparations, or procedures described herein.
Individual results vary, and no outcome can be guaranteed. This article reflects current understanding based on available research, but medical knowledge continually evolves. For personalized medical advice tailored to your specific situation, please consult with your healthcare team.
“`